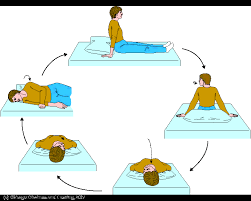
The widely adopted Epley maneuver, introduced by John Epley in 1992 ( 6, 7), has demonstrated efficacy and safety for PC-BPPV, with success rates ranging from 63.65 to 98% after one or more attempts ( 8).ĭespite its success, some patients exhibit poor response or canal switching, converting PC-BPPV to HC-BPPV during or after the maneuver ( 9). Treatment primarily revolves around repositioning maneuvers, aiming to relocate otoconia from the affected semicircular canal back to the utricle through a series of head movements ( 6). BPPV is further categorized based on the involved semicircular canal, with posterior canal BPPV (PC-BPPV) being the most prevalent, accounting for 80% of cases ( 4).ĭiagnosis relies predominantly on patient history and positional tests, such as the Dix-Hallpike test for PC-BPPV and the supine roll test for horizontal canal BPPV (HC-BPPV) ( 5). This migration disrupts normal endolymph flow and induces abnormal stimulation of the cupula ( 3). The prevailing pathophysiological understanding attributes BPPV to the detachment of otoconia from the utricular macula, migrating into one or more semicircular canals. Manifesting as brief episodes of vertigo and nystagmus, BPPV is triggered by alterations in head position relative to gravity, such as lying down, turning over, or standing up ( 2).

This study provides a new option for the treatment of BPPV.īenign paroxysmal positional vertigo (BPPV) stands out as a prevalent cause of peripheral vertigo, constituting 17–42% of reported cases ( 1). The BPPV virtual simulation model showed that the modified Epley maneuver could facilitate the passage of otoliths through the posterior arm of the posterior semicircular canal, especially through the location of obstruction.Ĭonclusion: The modified Epley maneuver is more effective than the traditional Epley maneuver in improving the single repositioning success rate and reducing the canal switching rate for PC-BPPV. Four cases in the control group experienced canal switching during the repositioning process, while none in the experimental group did. The experimental group achieved 100% repositioning success rate after two attempts, while the control group needed three attempts to reach 86% repositioning success rate.

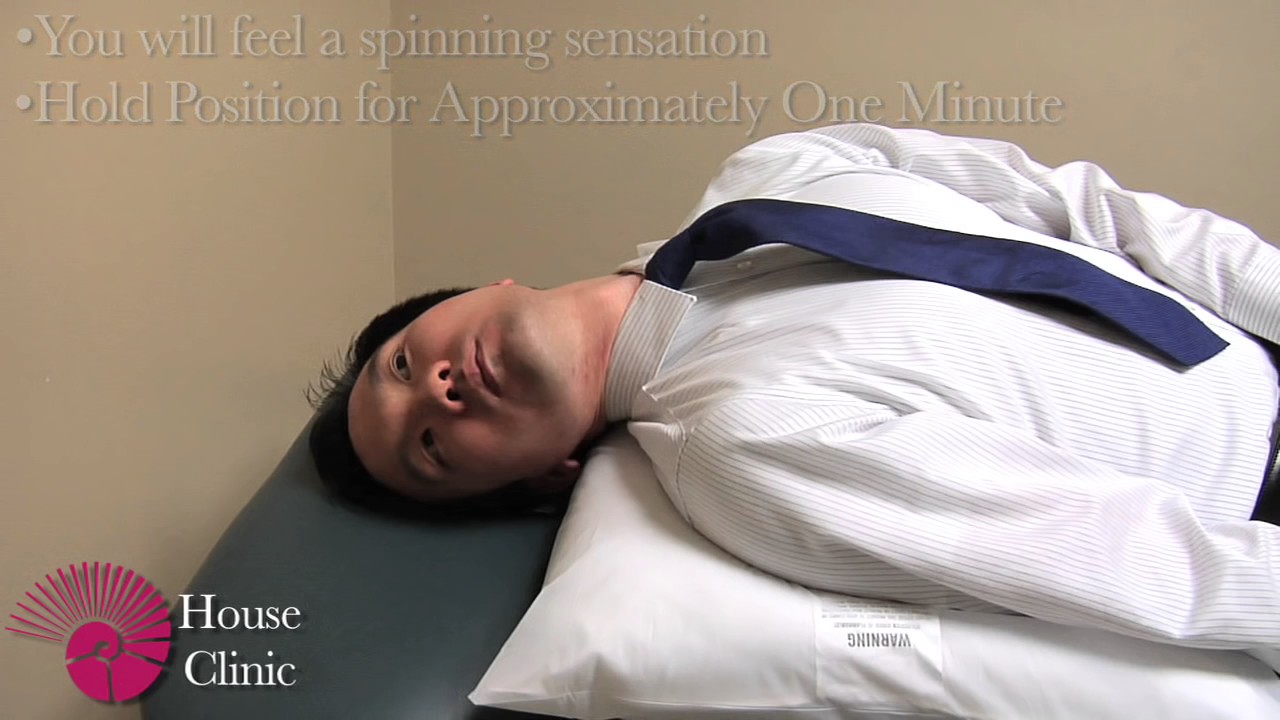
Results: The first repositioning success rate of the experimental group was significantly higher than that of the control group (85% vs. A BPPV virtual simulation model was used to analyze the mechanism of the modified Epley maneuver. The number of successful repositions after one, two, and three attempts and the total number of successful repositions were recorded and compared between the two groups. The control group received the traditional Epley maneuver, while the experimental group received the modified Epley maneuver, which prolonged the time in the healthy side lying position and the final bowing position. Methods: Sixty-five patients with unilateral PC-BPPV were randomly divided into two groups. Objective: To compare the repositioning effect of the modified Epley maneuver and the traditional Epley maneuver for posterior semicircular canal benign paroxysmal positional vertigo (PC-BPPV). 2Rehabilitation Department, Third Affiliated Hospital of Shanghai University, Wenzhou Third Clinical Institute Affiliated to Wenzhou Medical University, Wenzhou People’s Hospital, Wenzhou, China.1Neurology Department, Third Affiliated Hospital of Shanghai University, Wenzhou Third Clinical Institute Affiliated to Wenzhou Medical University, Wenzhou People’s Hospital, Wenzhou, China.Xiaosu Chen 1 † Jiesheng Mao 1 † Hua Ye 1 Luping Fan 2 Qiaowen Tong 1 Hehui Zhang 1 Chengcheng Wu 1 Xiaokai Yang 1 *
